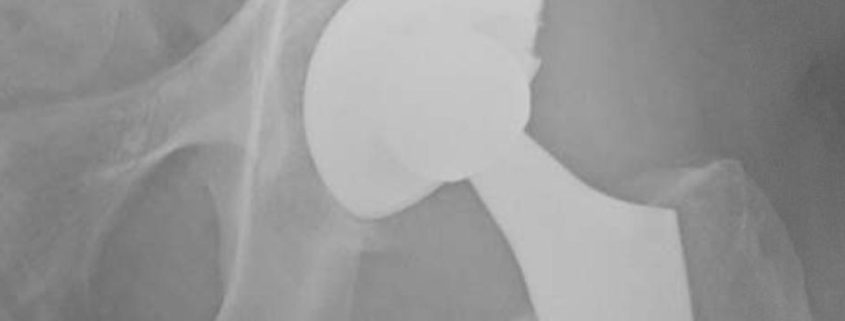
SuperPATH or Superior Approach To The Hip In Total Hip Replacement
Anterior Approach versus SuperPATH or Superior Approach in Total Hip Arthroplasty
I began using the superior approach for total hip replacement in February of 2014. This is a modification of the anterior and posterior approaches to the hip (its essentially an anterolateral hip approach deep but superficially the hip capsule is approached posterior to the gluteus medius and minimus).
The superior approach was originally described4, in 2004, by Stephen Murphy, MD, of the New England Baptist Hospital. The hip in this approach is never dislocated in the classical sense (intact head and neck rotated out of socket) – it must be removed piecemeal from the socket. This provides as close to a perfectly stable hip as one possibly could expect as the anterior and posterior capsule attachments to the femur are preserved. The only deep structure/muscle that is released is the piriformis tendon. This is subsequently repaired during closure. The dislocation rates quoted for this approach are in the 0.2-0.3% range, which is more favorable than the 0.6-0.7% range for the anterior and posterior approaches respectively. There is a variation of the “supercap” approach were a portal is used for acetabular reaming. This is described as a “superPATH” technique, or superior capsulotomy percutaneously assisted total hip. I’ve also seen this described as a Northern, a micro posterior, a direct posterior, or a direct lateral approach to address copyright issues.
PROS:
No dislocation performed so muscles, tendons, and capsule are only minimally stretched during removal of the cut femoral head. This means, in theory, less bleeding caused by the release and repair of the structures, and potentially less pain.
The only muscle structure occasionally released during the superior approach (also called the “supercap”, short for superior capsulotomy) – the piriformis tendon, is repaired in its natural position. The piriformis tendon is not able to be repaired with the anterior approach because after the tendon is released, it retracts posteriorly, out of the surgical field.
One of the reasons I have not used the anterior approach is due to anterior thigh pain experienced post-operatively from damage/stretching of the lateral femoral cutaneous nerve that supplies sensation to the anterior and lateral aspect of the thigh in 8-67% of patients (depending on what article you read2,3). Recently, an orthopedic surgeon wrote a candid report of his own experience after undergoing surgery having the mini-posterolateral approach on one side and anterior approach on the other.1 He preferred the mini-posterolateral because of the thigh pain experienced with the anterior approach. He is the joint replacement orthopedic surgery division head at Cooper University Hospital in Camden, NJ.
1Gordon Stuart L., A Tale of Two Approaches, Journal of Arthroplasty (2014), doi: 10.1016/j.arth.2014.01.028
2Bhargava T, Goytia RN, Jones LC, Hungerford MW, Lateral femoral cutaneous nerve impingement after direct anterior approach for total hip arthroplasty, Orthopedics (2010) Jul 13;33(7):472.
3Goulding K, Beaule PE, Kim PR, Fazekas A, Incidence of lateral femoral cutaneous nerve neuropraxia after anterior approach hip arthroplasty, Clin Orthop Relat Res (2010) Sept; 468(9);2397-2404.
4Murphy, Stephen B. “Technique of tissue-preserving, minimally-invasive total hip arthroplasty using a superior capsulotomy.” Operative Techniques in Orthopaedics 14.2 (2004): 94-101.http://www.stephenmurphy.org/hip/hminimally/101-107.PDF
http://www.stephenmurphy.org/hip/hminimally/murphy%20tissue%20preserving%20tha.pdf